Your shopping cart is empty!
|
|
|
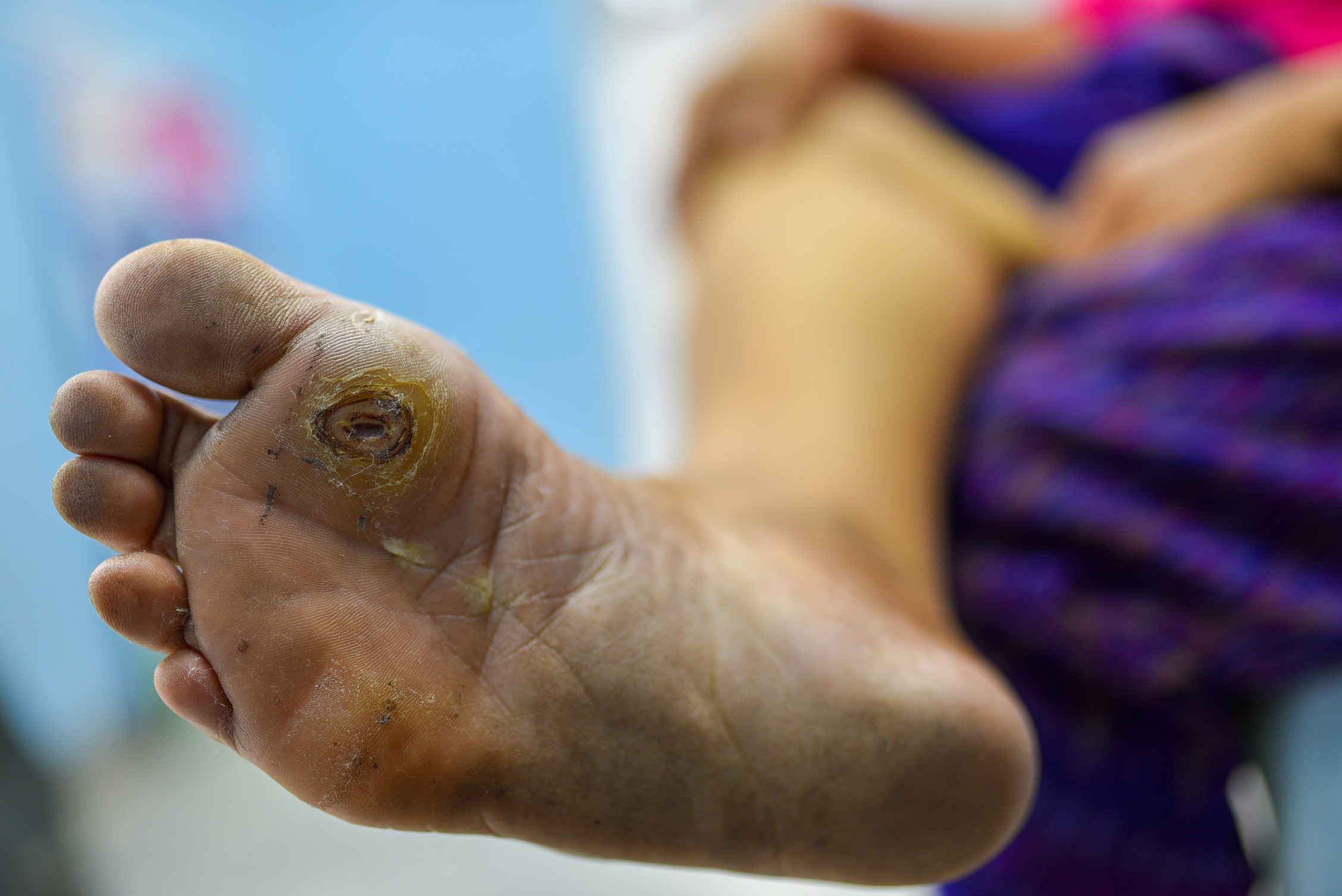
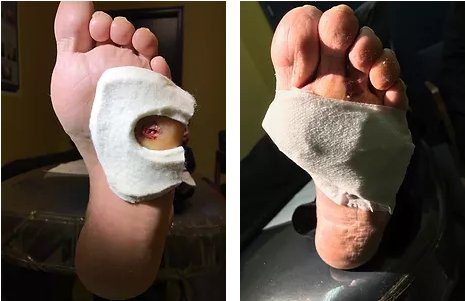
FORS Insole after 5 months daily usage:"The [FORS] innersoles are thicker than most, making offloading more effective. And they are quite well made. Adjacent plugs don't come loose and fall out, and these customizable insoles last a long time." Courtesy of Dr. S A Schumacher | Other brand after 1 month daily usage:"Some of these innersoles flatten out rather quickly, and adjacent plugs become loose and fall out...expanding the size of the desired hole, diminishing the effectiveness...doing nothing to offload the ulcer." Courtesy of Dr. S A Schumacher | Other brand after 2 weeks daily usage:"Not Made For Heavy People...It didn't take two weeks before it came apart...The FORS insole from Bonapeda is made of much sturdier stuff and has so far held out quite nicely." Courtesy of David Freeman, originally posted on amazon.com |
What Physicians Are Saying
"The FORS insole is easily modified to address patients, and is also very effective....It is made of rugged materials that will hold up and maintain offloading for a year...and it doesn't produce an 'edge effect'...It is a great insole, it just works...I really think it is the best of all the offloading insoles." DR. JAMES MCGUIRE, DPM, LPT. LPed. |
"...The FORS innersoles cost a bit more up front, but they offload better, so wounds close faster, meaning fewer overall visits and a lower complication rate, saving patients money in the long run. The FORS holds up as long or longer than 3 cheap innersoles, which are prone to flatten and break apart, putting more pressure back on the wound...The competition isn't even close." DR. S.A. SCHUMACHER, DPM, DABPS, DABPM, FAPWHc, FASPS, FACFAS, FACFAOM |
"When used in conjunction with utilization of a "team approach" and use of modern wound care techniques, I have found FORS to be a highly cost-effective option for plantar pressure reduction. It has shown to dramatically reduce the severity of wounds, decrease healing times, and reduce amputation rates." DR. PAYAM RAFAT, DPM, C.Ped |
"My 'go-to' is the FORS, which I use 90% of the time...It's stable and easy to put on...I like it and the patients like it...The FORS offloading insole should be of prime consideration when TCC isn't possible or practical, as well as for step down after TCC." DR. HARRY PENNY, DPM, AWPHc, FAPWHc |
"The FORS-15 system is easily customized for the patient, is not time consuming, is relatively inexpensive, and patient compliance is very high." DR. SCOTT PICKETT, DPM, FAPWHc |
PHYSICIAN INTERVIEWS ABOUT FORS™ (see more on our youtube channel) | |
|---|---|
INSTRUCTIONAL VIDEOS | |
| WHY FORS IS NEEDED NOW | |
I have not ever had as much help as I had with Bonaped. The insole works perfectly. Thank ya'll so much..
These are durable and high-quality heel lifts! Best I’ve used! ..
I have been using these for several years and they are excellent. I tried some of the cheaper brands but they just don't work as well. Deliv..
My job as a natural resource tech requires me to walk in the southwest desert outside Las Vegas conducting surveys. I walk anywhere from 2-1..
Try and put socks on and the zipper broke. Company issued a refund. Would work with them again...
Socks arrived promptly via US Postage from a different company, Stridelite. after one day of wearing the socks, which I liked very much, the..
This is a truly great product.. thank you so much..
Seems to be fine..
Perfect solution for Morton’s Neuroma. They are a perfect fit and very comfortable. Highly recommend this brand. ..
Excellent InsolesI have been using insoles for many many years and these are the best insoles I have ever used. They are highly recomm..